Most patients approach a hair transplant consultation focused on the recipient area—where the hair is going, what the hairline will look like, and how dense the result will be. These are reasonable priorities. But in donor area management, the factor that most determines whether a transplant delivers lasting results isn’t the recipient area at all—it’s the donor area.
Your donor supply is finite. There is no replenishing it. How it’s managed — in this procedure, and across every future procedure — is the foundation everything else is built on. A well-executed transplant that overspends the donor zone leaves you with a good result today and diminished options tomorrow. A well-planned transplant that treats the donor area as the long-term resource it is protects both. Contact Northwestern Hair Today for more information.
What the Donor Area Is and Why It Works
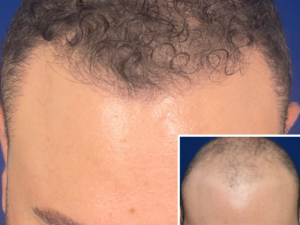
 The donor area — typically the back and sides of the scalp, running from above the ears across the occipital region — contains follicles that are genetically resistant to the DHT-driven miniaturization responsible for most hair loss. These follicles retain that resistance when transplanted. A hair that moved from the back of the scalp to the hairline grows there with the same DHT-resistant characteristics it had in its original location. This principle — donor dominance — is the biological foundation that makes hair transplantation work at all.
The donor area — typically the back and sides of the scalp, running from above the ears across the occipital region — contains follicles that are genetically resistant to the DHT-driven miniaturization responsible for most hair loss. These follicles retain that resistance when transplanted. A hair that moved from the back of the scalp to the hairline grows there with the same DHT-resistant characteristics it had in its original location. This principle — donor dominance — is the biological foundation that makes hair transplantation work at all.
It also explains why the donor area is irreplaceable. The resistance is in the follicle, not the location. Body hair and beard hair can sometimes supplement scalp donor hair in specific cases, but the scalp donor zone remains the primary and most reliable source. Once a follicle is removed from it, it’s gone from that zone permanently.
How Much Donor Hair a Patient Has
The total number of usable grafts available over a patient’s lifetime typically falls somewhere between 4,000 and 8,000, depending on hair density, shaft thickness, curl pattern, scalp laxity, and the extent of hair loss. These aren’t precise numbers — they’re a range that varies considerably from patient to patient, and that varies because the underlying variables vary.
Coarser or curlier hair generally provides better visual coverage per graft than fine straight hair, which affects how far the available supply can stretch. A patient with dense, coarse donor hair and moderate hair loss is working with a fundamentally different equation than a patient with fine hair and a strong family history of extensive loss. The consultation is where those variables get assessed and translated into a realistic picture of what’s achievable now and what should be held in reserve.
Strategic Graft Allocation
 The number of grafts used in a procedure matters. Where and how they’re used matters more.
The number of grafts used in a procedure matters. Where and how they’re used matters more.
The cosmetically critical zones — the hairline, the temples, the mid-scalp framing that most affects facial balance — are not equal in visual importance to the crown. A patient with limited donor supply who uses most of it filling the crown is making a trade-off that will likely look wrong in five years, as the hairline continues to recede while the crown stays dense. Strategic allocation means understanding the hierarchy of visual impact and sequencing the use of donor supply accordingly.
It also means reserving capacity. Hair loss is progressive. The plan built today has to account for the probability of future loss, which means not using everything available in the first session, even when the patient would prefer maximum immediate density. A surgeon willing to have that conversation honestly is protecting the patient’s long-term interests. One who isn’t is optimizing for the result that photographs best at twelve months.
Overharvesting: What It Is and Why It Happens
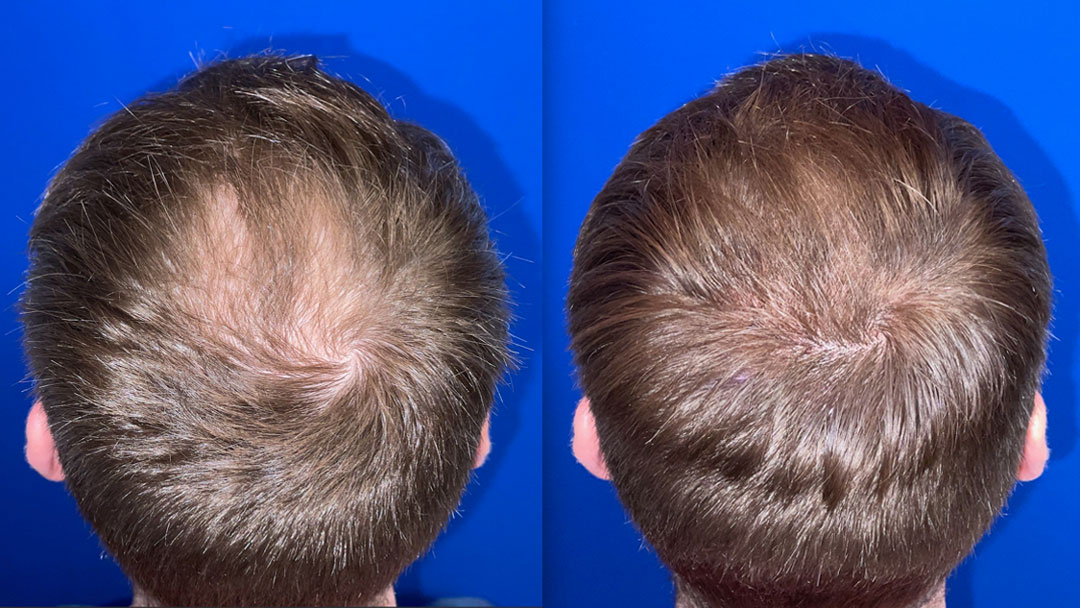
Overharvesting occurs when too many grafts are removed from the donor zone in too concentrated a pattern, leaving behind visible thinning, patchiness, or a texture sometimes described as moth-eaten. It’s one of the most common causes of poor long-term outcomes in hair restoration — and one of the most preventable.
It happens for a few reasons. High-volume clinics under pressure to deliver large graft counts in a single session may extract too densely from a limited area rather than distributing extraction evenly across the available zone. Surgeons without deep experience in donor management may not accurately assess the safe extraction threshold for a given patient’s density and coverage. And patients who push for maximum grafts without understanding the trade-off may be accommodated when they shouldn’t be.
The damage from overharvesting is permanent. The follicles that were removed can’t be returned, and the thinned donor area can’t be fully restored. Preventing it requires even distribution of extraction across the donor zone, appropriate spacing between extraction sites, accurate assessment of each patient’s safe yield, and a surgical team that understands the difference between what can technically be removed and what should be. When those conditions are met — and when technique is precise enough to minimize trauma at every extraction site — high-volume sessions become possible without compromising donor integrity. Micro PUE is what makes that achievable; the reduced follicular trauma at each extraction site is what allows the cumulative volume to scale without the donor area paying for it.
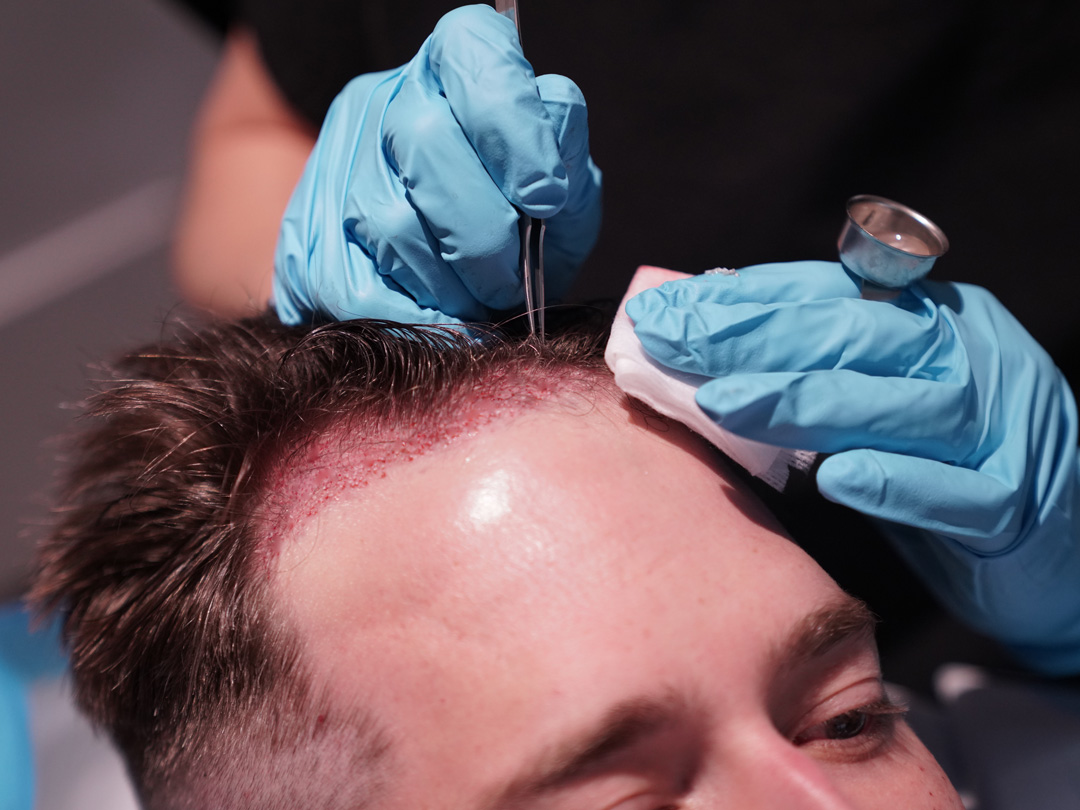
Extraction Technique and Donor Integrity
How grafts are extracted directly affects how the donor area looks afterward — and how much capacity remains for future procedures. Micro PUE, our refined approach to follicular extraction, uses precision instrumentation calibrated to minimize the mechanical trauma to both the extracted follicle and the surrounding tissue. The result is better graft survival on the recipient side and a donor area that heals cleanly and maintains its density for future use.
Even distribution of extraction across the available zone — rather than concentrating removal in a single area for convenience — is what keeps the donor region looking natural after healing. A donor area managed well is one that, at six months post-procedure, shows no visible sign that anything was taken from it.
Planning for Future Hair Loss
Hair loss doesn’t stop because a transplant was performed. The transplanted hair is permanent. The native hair surrounding it is not necessarily protected, and in many patients, it continues to thin over the years following the procedure. A plan that doesn’t account for that progression will eventually show it.
Long-term donor management means thinking about the patient’s hair at forty, fifty, and sixty — not just at twelve months post-procedure. That means maintaining a reserve in the donor zone for future sessions, designing hairlines that will still look age-appropriate as the surrounding hair evolves, and incorporating a medical maintenance strategy that slows the progression of native hair loss alongside the surgical work. The transplant and the long-term plan are not separate things. They’re the same conversation.
Donor Area Healing and Recovery
With proper extraction technique, the donor area heals predictably and without visible long-term signs of the procedure. In the first week, minor redness and scabbing at extraction sites are normal. By two to four weeks, healing is well underway, and the extraction sites become significantly less visible. By one to three months, the donor region typically looks entirely normal to anyone who doesn’t know to look closely.
Following post-procedure care instructions during the healing phase — particularly avoiding trauma to the donor area and adhering to washing and sun-exposure guidance — directly affects how cleanly and quickly the healing resolves.
What to Look for in a Clinic’s Approach to Donor Management
The way a clinic talks about donor management in a consultation tells you a great deal about how they approach the procedure as a whole. A provider who discusses graft allocation in terms of your full lifetime of options — not just today’s session — is thinking about your long-term outcome. A provider who promises maximum density without discussing the donor reserve trade-off is not.
Ask specifically how many grafts they estimate are available in your donor zone over your lifetime, how they determine the safe extraction threshold for a single session, and what they recommend holding in reserve. The answers will tell you whether you’re looking at a clinic that treats donor management as a serious clinical discipline or one that treats it as a logistical detail.
Schedule a Consultation at Northwestern Hair Restoration
If you’re considering a hair transplant and want to understand your true donor capacity—how many grafts are available, how they should be distributed over time, and what a responsible long-term plan looks like—Donor Area Management is where that conversation begins. A consultation with Dr. Vinay Rawlani focuses early on this assessment, because it forms the foundation for every decision that follows.
In-person evaluations are available at our Chicago clinic. Virtual consultations are available for patients anywhere.